Heel pain is one of the most common diagnosis that we see in our practice. Heel pain is often due to an inflamed ligament on the bottom of the foot called the plantar fascia. Heel pain may also be due to other causes, such as a stress fracture, tendonitis, arthritis, nerve irritation, or, rarely, a cyst.
Because there are several potential causes, it is important to have heel pain properly diagnosed. As foot specialists we are able to distinguish between all the possibilities and determine the underlying source of your heel pain.
What Is Plantar Fasciitis?
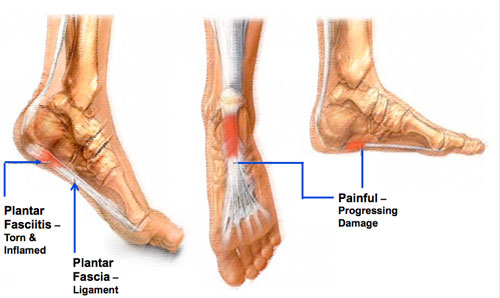
Plantar fasciitis is an inflammation of the band of tissue (the plantar fascia) that extends from the heel to the toes. In this condition, the fascia first becomes irritated and then inflamed, resulting in heel pain.
Causes
The most common cause of plantar fasciitis relates to faulty structure of the foot. For example, people who have problems with their arches, either overly flat feet or high-arched feet, are more prone to developing plantar fasciitis.
Wearing non-supportive footwear on hard, flat surfaces puts abnormal strain on the plantar fascia and can also lead to plantar fasciitis. This is typically found when one’s job requires long hours on the feet. Obesity may also contribute to plantar fasciitis.
Symptoms
People with plantar fasciitis often describe the pain as worse when they get up in the morning or after they’ve been sitting for long periods of time. After a few minutes of walking the pain decreases, because walking stretches the fascia. For some people the pain subsides but returns after spending long periods of time on their feet.
Diagnosis
To diagnose the type of heel pain that you suffer from our staff will obtain your medical history and examine your foot. Throughout this process our foot specialists will rule out all the possible causes for your heel pain other than plantar fasciitis.
In addition, diagnostic imaging studies such as x-rays or other imaging modalities may be used to distinguish the different types of heel pain. Sometimes heel spurs are found in patients with plantar fasciitis, but these are rarely a source of pain. When they are present, the condition may be diagnosed as plantar fasciitis/heel spur syndrome.
Non-Surgical Treatment
- Stretching exercises
- Avoid going barefoot.
- Ice.
- Limit activities.
- Shoe modifications.
- Medications.
If you still have pain after several weeks, our foot specialists, will add one or more of these treatment approaches:
- Padding and strapping. Placing pads in the shoe softens the impact of walking. Strapping helps support the foot and reduce strain on the fascia.
- Orthotic devices. Custom orthotic devices that fit into your shoe help correct the underlying structural abnormalities causing the plantar fasciitis
- Injection therapy. In some cases, corticosteroid injections are used to help reduce the inflammation and relieve pain.
- Removable walking cast. A removable walking cast may be used to keep your foot immobile for a few weeks to allow it to rest and heal.
- Night splint. Wearing a night splint allows you to maintain an extended stretch of the plantar fascia while sleeping. This may help reduce the morning pain experienced by some patients.
- Physical therapy. Exercises and other physical therapy measures may be used to help provide relief.
When Is Surgery Needed?
Although most patients with plantar fasciitis respond to non-surgical treatment, a small percentage of patients may require surgery. If, after several months of non-surgical treatment, you continue to have heel pain, surgery will be considered. Our foot specialists will discuss the surgical options with you and determine which approach would be most beneficial for you.
Minimally invasive surgical procedures for Chronic plantar fasciitis
1) Shockwave Therapy (EPAT)
WHAT IS EPAT THERAPY?
EPAT therapy is a highly effective treatment method: high-energy sound waves are introduced into the painful areas of the body. It is one of the most advanced and highly effective noninvasive treatment methods cleared by the FDA. The treatment works by helping to improve the regenerative potential, enhancing blood circulation to regenerate damaged tissue.
EPAT also known as Shockwave and Pressure Wave Therapy can successfully address all musculoskeletal pains and injuries of of the foot and ankle inlcluding plantar fasciitis/heel pain, achilles tendonitis, turf toe, stress fractures, Posterior tibial tendonitis, and other tendonitis in the foot and ankle.
Treatments typically take about 5-10 minutes, depending on the disorder being treated. Generally 3 treatments are needed each about 1 week apart. The benefits are often seen after only 3 treatments with some patients experiencing immediate pain relief. The non-surgical therapy for pain eliminates pain and restores mobility, thus quickly improving patients’ quality of life.
Call us to learn more about how EPAT Therapy can address your pain, accelerate your healing and optimize your health.
BENEFITS OF EPAT TREATMENT
- 91% Success Rate (as per clinical studies)
- Non-invasive
- No anesthesia required
- No risk of infection
- No scarring
- No downtime
- Over 80% patient satisfaction
- Cost effective
- Faster, easier healing
FREQUENTLY ASKED QUESTIONS
Q: What is EPAT Technology?
ANSWER:
EPAT is a non-invasive modern and highly effective treatment method: high-energy sound waves are introduced into the painful areas of the body. Pressure wave technology accelerates the healing process in the body by stimulating the metabolism and enhancing blood circulation to regenerate damaged tissue. Strong energy pulses are applied to the affected area. These pulses occur for short periods of time, creating micro-cavitation bubbles that expand and burst. The force created by these bubbles penetrates tissue and stimulates cells in the body that are responsible for bone and connective tissue healing.
Q: What type of conditions can be treated with EPAT Technology?
ANSWER:
EPAT treatment can successfully address acute and chronic pain such as: Knee Pain, Heel Pain , Foot Pain, Ankle Pain, Hamstring Pain, Back Pain, Neck Pain, Shoulder Pain , Elbow Pain, Wrist Pain and Hand Pain and much more.
Q: How is the treatment performed?
ANSWER:
EPAT treatment is noninvasive. Gel is applied to the treatment area; pressure waves are then released through the applicator as it is moved over the treatment area.
Q: How many treatments are generally needed?
ANSWER:
The number of sessions needed depends on the condition that is being treated. Each treatment session takes between 10-15 minutes and can vary depending on the condition that is being treated.
Q: What type of results are expected?
ANSWER:
Beneficial effects are often experienced after only 1 or 2 treatments and there is no downtime. Many patients report immediate pain relief after treatment. The technology has a 91% success rate as per clinical studies, patients treated report being pain free and /or have a significant reduction in pain. The non-surgical therapy for pain eliminates pain and restores mobility, thus improving patient’s quality of life
Q: What are the possible side effects?
ANSWER:
Treatment with EPAT technology has virtually no side effects. In some cases, patients may experience minor discomfort for a few days. Patients can return to work after treatments and in most all cases there is no down time
Q: Who is a candidate for EPAT?
ANSWER:
Most people are good candidates for EPAT treatment however patients who are pregnant, have a pacemaker or current cancer are not suitable for treatment with EPAT Technology. Your doctor will provide you with information about conditions you may have that would affect your ability to undergo treatment.
Q: How can learn if EPAT Treatments will help my condition?
ANSWER:
Please call our practice at:
Carolina Foot & Ankle Specialists
West Ashley location: (843) 225-5575 Dr. Adam Brown
Mt. Pleasant location: (843) 654-8250 Dr. Andrew Saffer
We have experienced staff that can answer your questions and make an appointment for you to come in for a consultation visit.
2) Topaz
Our foot specialists have been performing the Topaz procedure since 2006. Originally, the procedure required an incision. The procedure is an outpatient surgery under mild sedation and local anesthesia. A series of needle holes are made into the plantar fascia region of pain and the Topaz probe is inserted and used to break up the scar tissue through a large burst of heat and energy. micro fascia releases break up the scar tissue and release the fascia in a microscopic level that allows for healing and less pull of the fascia on the heel. This is what we refer to as a micro plantar fascia release. No sutures are required.Recovery is about 4-6 weeks. Patient's are placed in a boot for one week and then sneaker one week after the procedure. Physical therapy may be necessary to decrease pain and help with healing.
3) Instep plantar fasciotomy
The in-step plantar fascia release is used in cases of a severely tight plantar fascia that has pain associated with the heel and possibly the arch region. An instep arch plantar fascia release allows release of the fascia in the tightest region and the incision is made in a non-weight-bearing region of the foot. The procedure is done in outpatient hospital or surgery center under sedation. An incision is placed in the arch region and the fascia is released in its arch side only. The outer side of the fascia is left intact to support the outside portion of the foot while the arch portion, which is normally tight, is released. The patient is allowed to put weight on the foot right after surgery in a boot and is kept in the boot for about 3-4 weeks. Return to full activity, which is expected to take 6-8 weeks in total from the time of surgery.


